Research
Over two decades of innovative research
and care ministry.
Our approach to research involves community stakeholders engaging as partners in all steps of the research process with the goals of educating, improving practice, or bringing about changes in social determinants.


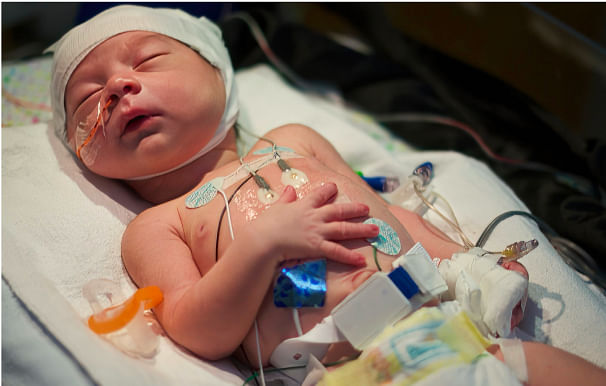


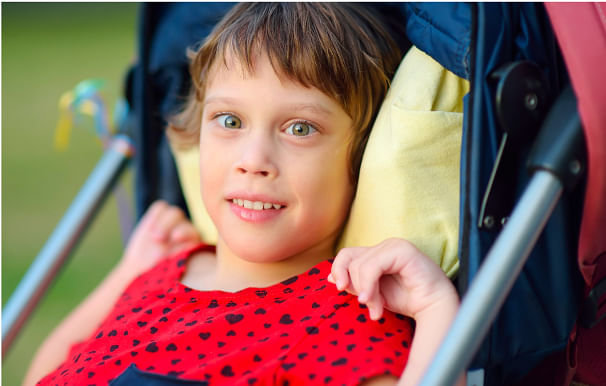
RIGHTCARE’S collaborative approach to research involves stakeholders throughout the research process. We use a research framework that aims to address the practical concerns of people in a community. The framework begins with a community’s issue, proposed action or strategy, and then supports or enhances this action with research that is community based and engaged. By its nature, our research is applied research; it seeks to change issues that are critical to communities and focuses on engaging community members in research directed at addressing their needs and concerns.

Current Projects
We are continuously engaged in research tied to achieving outcomes for seniors. Below are a sample of projects we are currently engaged in:
Medical equipment and supplies are essential in maintaining life, fostering progress, and averting further deterioration in medically complex children. Durable Medical Equipment (DME) and supplies are as pivotal as any aspect of the care plan in enabling these children to reach their utmost potential. Frequently, it is the key factor that allows for their return home. However, the process of prescribing, obtaining, and using adaptive equipment and supplies is more complex than it appears. This complexity arises due to the vast array of available equipment, complexity of the children, and the often-underestimated multitude of factors that influence the optimal selection, procurement, and use of equipment for each child in their home environment. Pediatric clinicians analyze critical information to determine why a child is having difficulty and intervene to increase the child’s potential for success. One key intervention they use to help achieve success is the integration of durable medical equipment and supplies. Neglecting to provide the necessary and optimal devices and supplies (variances and omissions) can have significant and often detrimental effects on both the child and their family. Such oversights not only risk the child's well-being but also result in adding stress to necessary tasks, as well as a loss of valuable time that could have been better spent on tailoring equipment and training more closely aligned with the child’s specific needs. Problem Overview There is a staggering 100% variance and omission rate when providing optimal and necessary equipment and supplies for medically complex children. Meaning that when a child is either leaving the hospital or is already at home, 100% of the time there is one, or more, variances and/or omissions with their equipment and supplies. On average, the number is twenty-six. This alarming statistic indicates that nearly all such children are not receiving the equipment, supplies, or training they need, or are receiving less effective or incomplete solutions. This gap not only compromises the effectiveness of the care they require but also hinders their ability to achieve their best possible quality of life. The failure to equip these children with the right tools tailored to their specific needs greatly impacts their development, independence, and overall health, while often significantly adding unnecessary burden and stress to family caregivers. Moreover, this high rate of variance and omission is due to systemic flaws in the assessment, prescription, procurement, and delivery processes of medical equipment, calling for urgent attention and improvement to ensure that these vulnerable children receive the care and support they truly need. A comprehensive analysis conducted on the variance and omissions in the provision of equipment for medically complex children revealed a concerning lack of fundamental methodology in the needs assessment process. This analysis, which scrutinized a wide range of cases (n=7,021), uncovered a consistent pattern. The approaches used to determine the equipment and supply needs of these children were not only inadequate but also lacked a standardized, evidence-based framework. The correlation between the high rates of variance and omissions and the flawed assessment methodologies was striking. This lack of a robust, systematic approach in evaluating the specific requirements of each child led to frequent mismatches between the prescribed equipment and supplies and the actual needs, severely impacting the effectiveness of care and intervention strategies. Further, the analysis highlighted that the existing assessment processes were often superficial and did not account for the complex, multifaceted needs of these children. This oversight resulted in a one-size-fits-all approach, which failed to cater to the unique needs of each child. The findings of this analysis underscore the urgent need for a more comprehensive, individualized, and methodologically sound approach in the needs assessment for medical equipment, to ensure that these vulnerable children receive the most appropriate and effective support for their development and well-being.
Nationally, there are millions of non-fatal falls requiring medical attention each year. These non-fatal falls account for hundreds of millions of dollars in emergency response alone and account for over 8 million DALYs (disability adjusted life years) lost. The largest morbidity occurs in people aged 65 yeas and older.
While large amounts of research has been done on falls over the last 20 years, its prevalence nationally, on senior campuses, and in local communities continues to rise year over year. A careful examination of the information surrounding falls reveals a repeating discussion of the same general contributing factors and limited options to deal with them. The unabated rate of falls within the existing senior population shows that no effective solutions or responses have been developed from understanding these large generic factors.
On the front lines dealing with the results of this epidemic is our dedicated EMS and Fire Department personnel. A review of the literature put out by fire department and EMS organizations shows discussion of the same problems faced across the country. Additionally, there are numerous secondary problems associated with responding to this epidemic of “lift assist” and “non-emergency” calls such as increased response times to overlapping calls and lack of funding for critical departments needs. No one has yet made a meaningful impact on the problem or changed the conversation locally. It appears that if this problem is going to be solved, it will have to be led by FD/EMS services. This project is a major step forward in solving this challenge.
In the search for understanding key levers to success, it is becoming clear that the current systems in place are not working. The general understanding of seniors who are at risk for “lift assist” and “non-emergency” calls has not generated effective solutions. Effective being defined as a sustained, cost effective, duplicatable programming that decrease the per capita number of lift assist and other preventable calls experienced within this population.
A senior person calling for a “lift assist” or other unsafe occurrence results from a specific and unique set of risks that caused them to have the unsafe occurrence leading to the call. In a majority of the cases, the senior’s pre-call scores have already over indexed in key areas to cause the crisis. If these key areas are not understood, measured, and improved, then it follows that another event necessitating emergency care or hospitalization will occur, whether or not there are additional risk factors resulting from the previous fall or crisis. Research has proven current solutions (social programs, home health, family involvement, clinician) when brought in to support change are unable to score these individual factors or effectively deal with them, resulting in continued risk of failure. Without clear understanding of these individual factors facing at risk senior populations, seniors are at risk of escalating frequency, types, and severity of unsafe occurrences.
Research suggests that the inadequacy of the demographic and medical record data on hand to provide a clear means to achieve outcomes and manage costs, fire departments, healthcare systems, and providers are hitting the ceiling of what they can do with current information sets. These poorly defined individual specific social-demographic-environmental-patient factors and behaviors appear to be where the majority of the causes for “non-emergency” and “falls and calls” and lie. So what are these factors causing such an enormous number of assists locally and nationally, and can they be defined and measured? If these individual factors could be identified, what would effective solutions look like that could adequately address them? What if it is this lack of awareness and understanding of specific factors, as well as a lack of effective follow up care that is setting up the next tragic event, ED visit, or hospitalization?
Goal
This goals of this collaborative are to: (1) quantify, for the first time in the country, the individualized (mSDOH) risk profile of the senior “fall assist,” and frequent caller, (2) quantify the deployment of necessary and effective resources for at risk seniors, (3) measure reduced follow up “lift assists,” and other preventable calls, (4) use education to promote awareness of the program to seniors and their adult children as evidenced by increasing the number of seniors/families who seek collaboration proactively, (5) measure the subjective experience of the seniors and family.
For this project a PBHS mSDOH model, LIFE Profile, (Lifestyle Feasibility Profile), is being used for client assessment and care plan development. The assessment delivers new data sets for care planning to maximize the value and benefit of in-home services. Scoring and outputs collected from the LIFE Profile assessment will deliver a care plan which is comprehensive, individualized, goal driven, and define individual and shared responsibilities for all participants that are involved in achieving care outcomes.
Scope 196 locations, 42 states, expected N=23,000.

Kurt Merkelz
RIGHTCARE Senior Board Member
Healthcare Division
Kurt Merkelz, M.D., is senior vice president and chief medical officer of Compassus and has been in this role since 2017.
Throughout his career, Merkelz has focused on caring for older adults. His perseverance in raising industry benchmarks for quality hospice care earned him the Compassus R. Sean Morrison, M.D., Award for Outstanding Achievement in Hospice Physician Leadership. He is currently serving a third term as co-chair for the National Quality Forum (NQF)’s Measure Applications Partnership (MAP) post-acute workgroup. Dr. Merkelz pioneering work in standardized care delivery garnered Compassus national recognition by NQF in 2020. Merkelz serves on several national organization committees including AAHPM, AMDA, and NHPCO.
Merkelz is triple-board certified in hospice and palliative care medicine, family practice and geriatrics.

Randy Bartosh
President, Performance Based Healthcare Solutions,
RIGHTCARE Board Member, RC Projects Leader
Randy is the head of research for PBHS (Performance Based Healthcare Solutions) which he founded in 1999.
Over the course of the last twenty two years Randy has led applied research collaboratives with 300+ care organizations involving over 75,000 senior lives. The research has been focused on categorizing, quantifying, and achieving the outcomes seniors need in order to be successful. His direct work has led to standardized care and care delivery models used in over 39 states in the U.S. as well as Canada and Australia. You will find him either leading integration projects, performing care visits for his local churches, or with his wonderful family playing along the Texas Gulf Coast where they live.